A London urologist’s guide to frequency, urgency, weak flow and nocturia
Urinary symptoms can creep in gradually — a weaker flow, waking at night (nocturia), rushing to the toilet (urgency), or going far more often than you used to. For many men, these issues are inconvenient and embarrassing, but they’re also clinically important because bladder symptoms can overlap with prostate enlargement, infection, overactive bladder, kidney stones, and (more rarely) urological cancers.
This confidential, informative guide is written for men in London and surrounding counties (Essex, Kent, Surrey, Hertfordshire, Buckinghamshire) and explains what symptoms can mean, when to get assessed, which tests are commonly used, and what modern treatments London urology services can offer.
The most common urinary symptoms in men (and what they can indicate)
Frequent urination (daytime frequency)
Needing to pass urine more often can be caused by:
- Bladder irritation (caffeine/alcohol, inflammation)
- Overactive bladder
- Infection (UTI)
- Diabetes/metabolic factors
- Incomplete emptying (often linked to prostate obstruction)
Urgency (the sudden “can’t wait” feeling)
Urgency is often seen in overactive bladder and bladder irritation, but it can also happen when the bladder is working harder due to obstruction.
Weak urine flow / hesitancy / stopping and starting
A weak stream or difficulty starting is commonly associated with benign prostate enlargement (BPH/BPE) and lower urinary tract symptoms (LUTS).
Nocturia (waking at night to pass urine)
Nocturia can be related to:
- Prostate/bladder outflow issues
- Overactive bladder
- Evening fluid intake, caffeine/alcohol
- Sleep disturbance, some medications, or wider medical factors
Lifestyle changes can help some men (especially reducing late fluids and bladder irritants such as caffeine).
Urinary tract infections (UTIs)
UTIs can cause frequency, urgency, burning pain, smelly/cloudy urine, and lower abdominal discomfort. Recurrent UTIs (for example, repeated episodes across months) should be assessed properly rather than repeatedly self-treating.
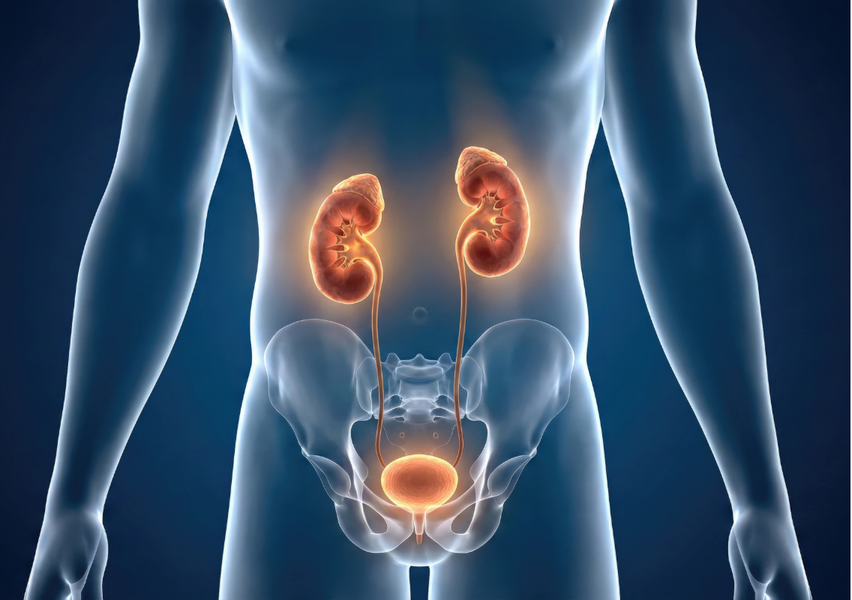
Why bladder symptoms often overlap with the prostate and kidneys
Prostate link (LUTS / BPH)
In middle-aged and older men, symptoms are commonly due to bladder outflow obstruction from BPH/BPE — but a proper assessment checks for other bladder causes too.
Kidney link (stones / obstruction / infection)
Kidney stones can sometimes mimic bladder symptoms — especially if a stone irritates the bladder as it moves lower, causing frequency/urgency or blood in the urine. Imaging (often CT in adults with suspected renal colic) is used to confirm stones.
When professional assessment is needed (don’t wait on these)
Seek medical assessment promptly if you have:
- Visible blood in the urine (haematuria), especially if unexplained or persistent after treating a UTI — this usually needs urgent urology assessment under suspected cancer referral guidance.
- Fever, flank/back pain, or feeling very unwell with urinary symptoms (possible kidney infection or obstructing stone)
- Inability to pass urine (acute retention)
- Recurrent UTIs or persistent symptoms despite treatment
What a urology assessment in London typically includes
A good assessment is structured and aims to find the cause, severity, and safest treatment route.
Common elements include:
- Symptom review (including a symptom score and “what bothers you most”)
- Medication and lifestyle review
- Examination where appropriate
- Urinalysis (dip test) and urine culture when infection is suspected
- Blood tests when indicated (kidney function, infection markers, PSA depending on age/risk and pathway)
NICE CKS outlines core assessment and investigation steps for men with LUTS, including when to consider referral and further tests.
Key diagnostic tests (and what they show)
Depending on your symptoms, your urologist may recommend:
- Urine tests (infection, blood, inflammation markers)
- Urine flow test (uroflowmetry) and post-void residual (to check flow strength and whether the bladder empties properly)
- Ultrasound (kidneys/bladder, residual urine, stones, hydronephrosis)
- CT scan if kidney stones are suspected (often urgent low-dose non-contrast CT in adults with renal colic)
- Cystoscopy (a camera test of the bladder) when indicated — especially with blood in urine or persistent unexplained symptoms
- Bladder diary / frequency-volume chart when overactive bladder is suspected (helps pinpoint urgency/frequency patterns)
Lifestyle and self-care that genuinely helps (not just generic advice)
For many men, small changes reduce urgency and nocturia:
- Reduce caffeine and alcohol (common bladder irritants)
- Avoid large volumes of fluid late evening (nocturia)
- Manage constipation (constipation can worsen bladder symptoms)
- Weight management and activity (can help urinary control and overall bladder function)
If symptoms are persistent or progressive, lifestyle changes are helpful — but not a substitute for proper assessment.
Advanced treatments available through London urology services
Treatment depends on the cause (prostate obstruction, overactive bladder, infection, stones, etc.) and your priorities (symptom relief, preserving ejaculation, avoiding long-term medication, and so on).
For prostate-related weak flow and obstruction (BPH/BPE)
Medication options may help many men before surgery is considered.
Procedures (for suitable patients), including:
- TURP (a common surgical option for enlarged prostate)
- HoLEP and other laser options (varies by centre)
- UroLift (minimally invasive implants to open the channel in selected men)
- Rezūm (steam ablation; tissue shrinks over months; often day-case in appropriate men)
For overactive bladder (urgency, frequency, urge leakage)
Conservative measures (bladder training, lifestyle changes) are typically tried first; medications may be used when symptoms persist. NICE guidance and NICE technology appraisal evidence support antimuscarinics as a usual first pharmacological option, with mirabegron as an option when antimuscarinics are unsuitable or ineffective.
For UTIs and recurrent infection patterns
Treat the infection appropriately and investigate why it’s happening (for example, incomplete emptying due to obstruction). Recurrent or persistent UTIs warrant GP/urology review.
For stones and kidney-related causes
Imaging confirms diagnosis, then treatment is based on stone size/location and symptoms. NICE sets out CT as first-line imaging for adults with suspected renal colic (unless contraindicated, e.g., pregnancy).